Chondrosarcoma: History, Clinical Aspects, Classification, Differential Diagnosis, Treatment, Complication and Prognosis
– primary tumors of the bones
– tumors developed in pre-existing bone lesions
– tumors resulting from ionizing radiation
– tumors that invade the bones, originating from soft tissues
– primary tumors of the joints
– metastatic tumors in the skeleton 23 .
In 1925, Keiller and later Phemister, 1930, were the first to separate chondrosarcoma from osteogenic sarcomas, considering the distinction between their morphological and clinical-radiological characteristics, as well as their slower evolution and better prognosis. In 1939 the “Committee of the bone sarcoma registry” included chondrosarcoma as a distinct entity.
Lichtenstein and Jaffe, in 1943, established a clear distinction between osteosarcoma and chondrosarcoma. Osteosarcoma is a tumor that produces neoplastic osteoid, while chondrosarcoma occurs from fully developed cartilage, often presenting calcification or ossification, but never producing neoplastic osteoid 2 .
Definition : Chondrosarcoma is a malignant neoplasm of mesenchymal nature, producing interstitial substance and cells that take on the appearance of hyaline cartilage, with varying degrees of immaturity and frequent foci of calcification. It is the most common primary malignant lesion of the bone after osteosarcoma 23,24 and Ewing’s tumor (silabus), it can affect any age, with a predominance between 30 and 40 years 7,11,22 , with reports in the literature between three and 73 years 15 .
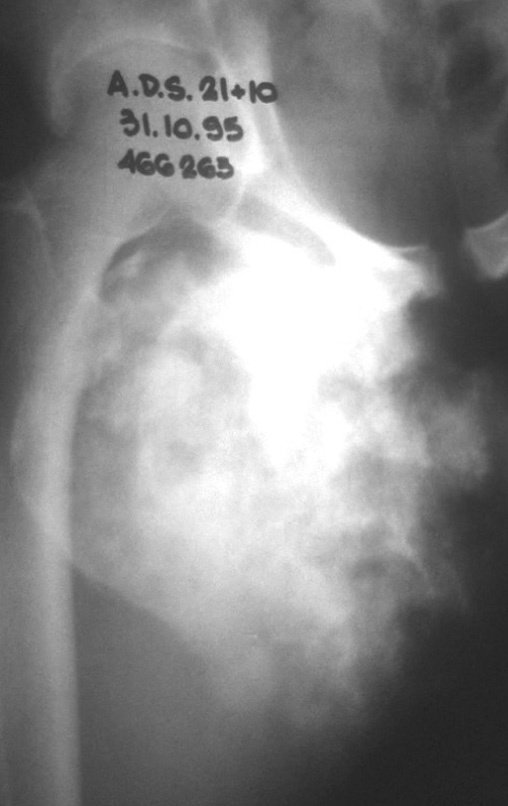
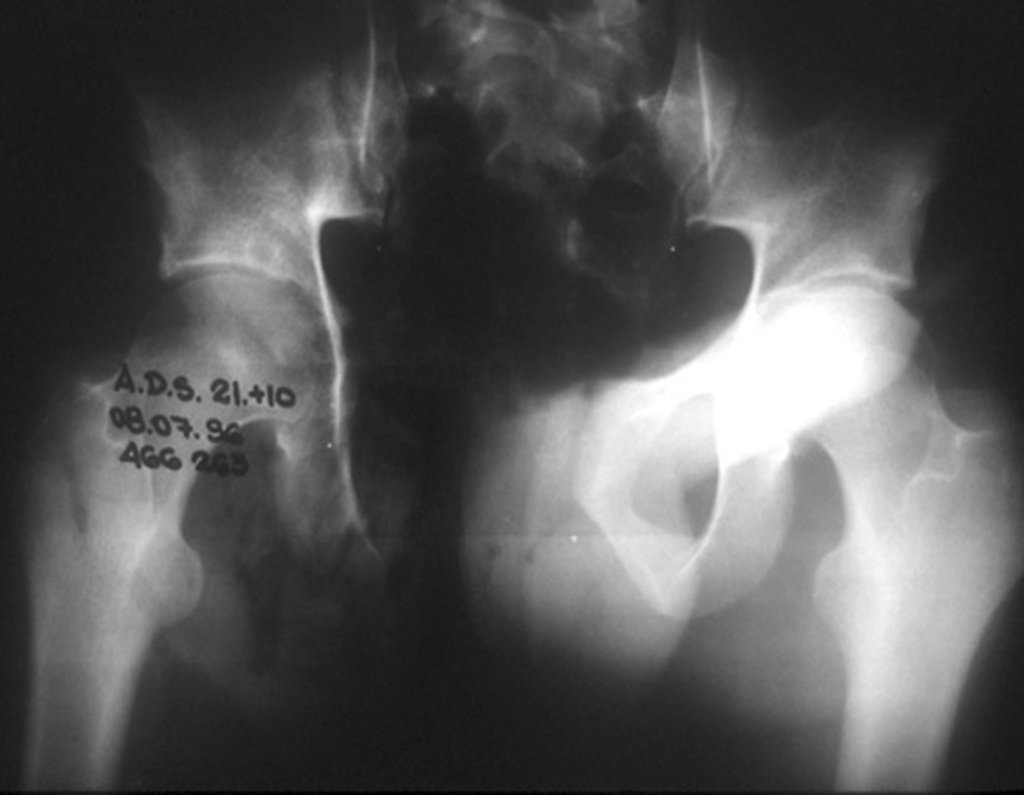
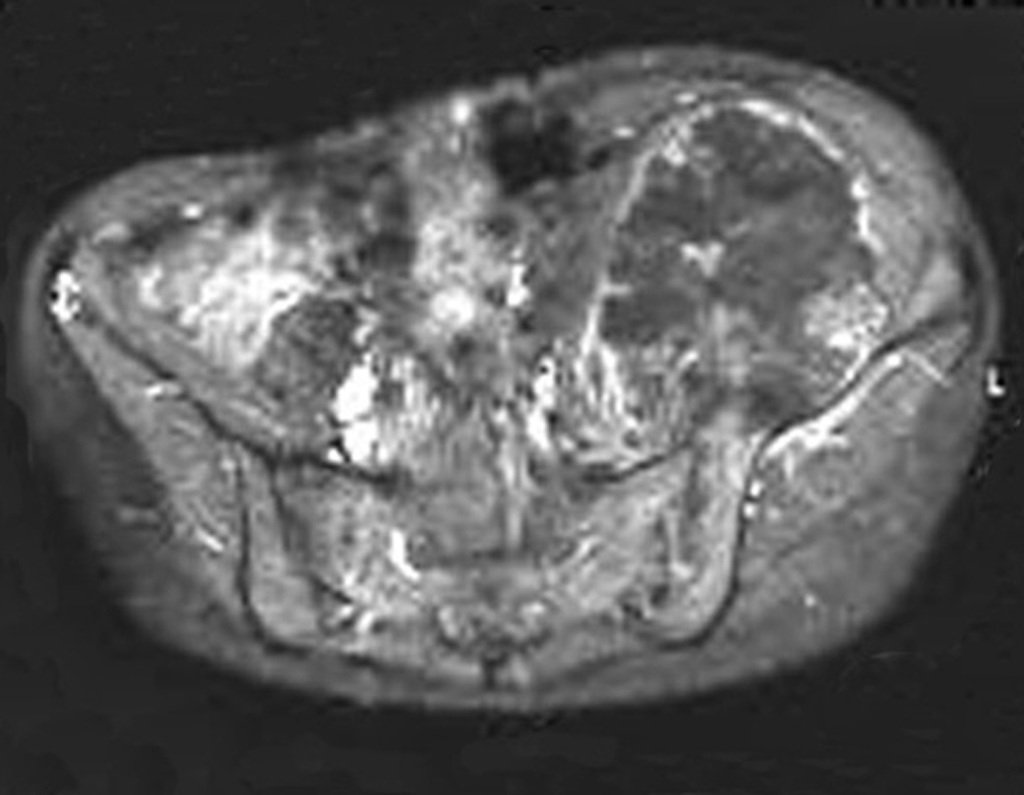
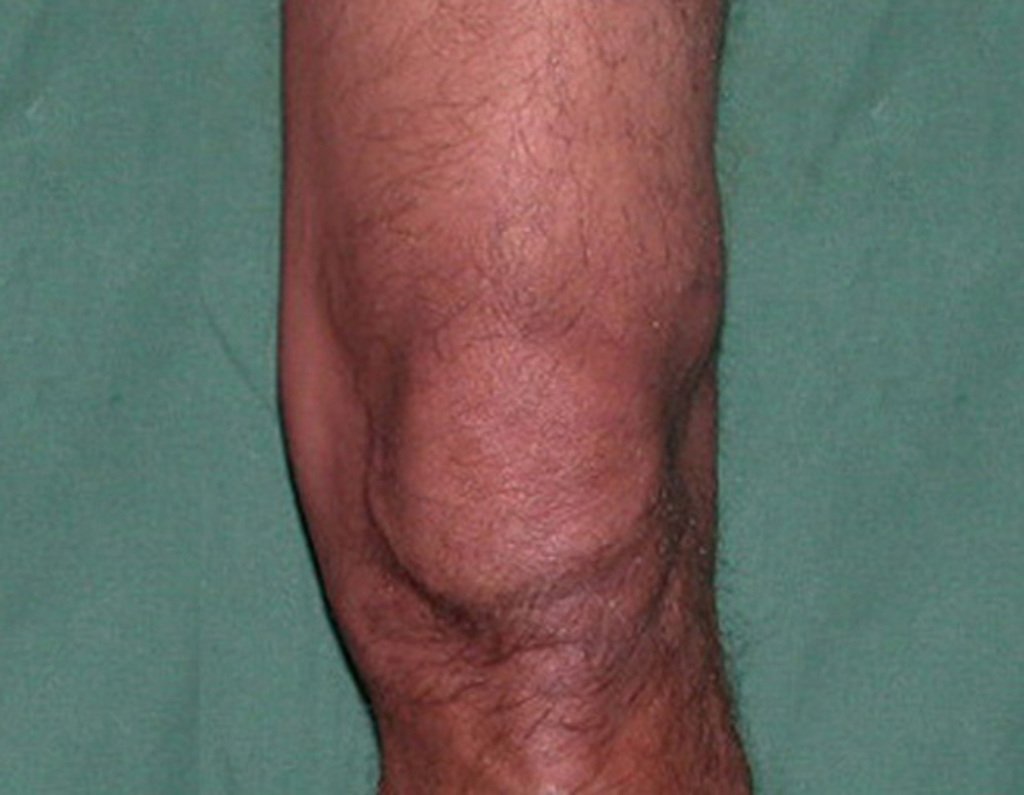
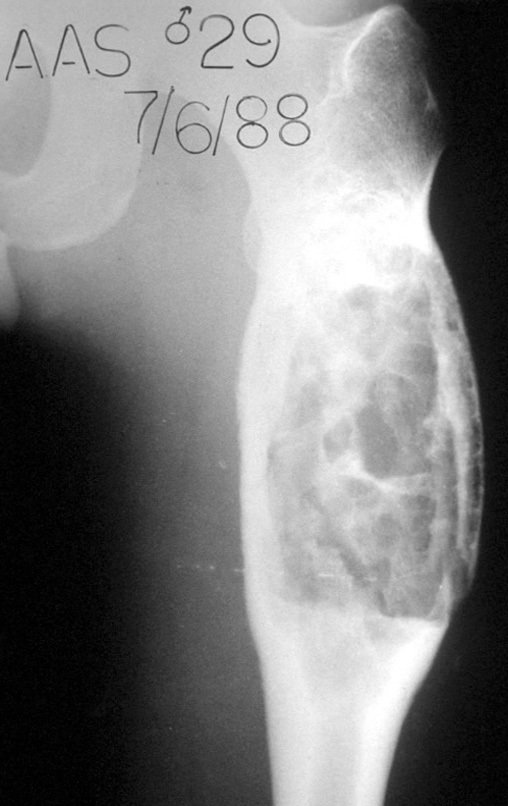
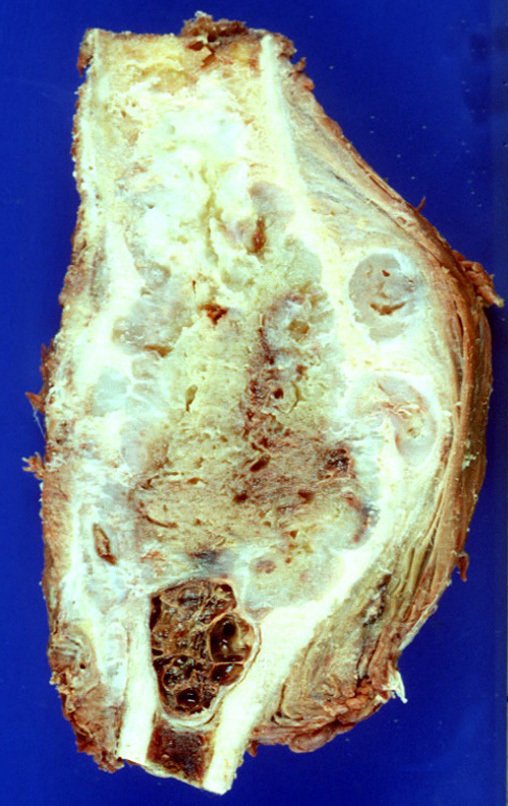
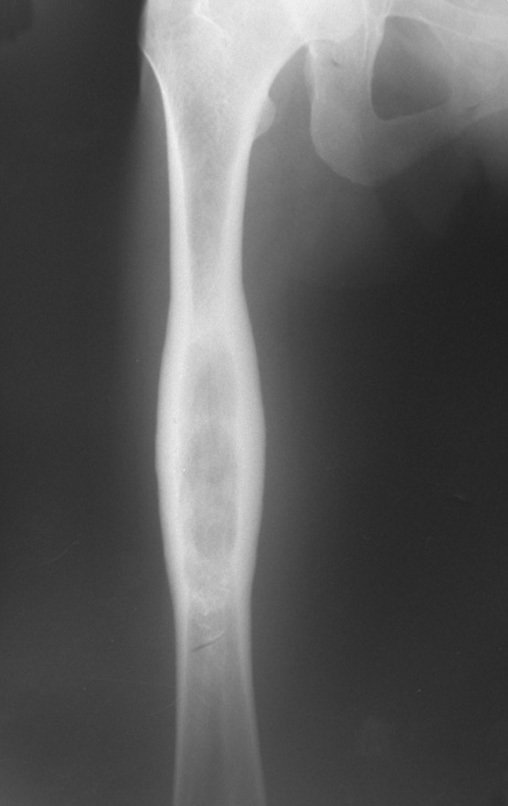
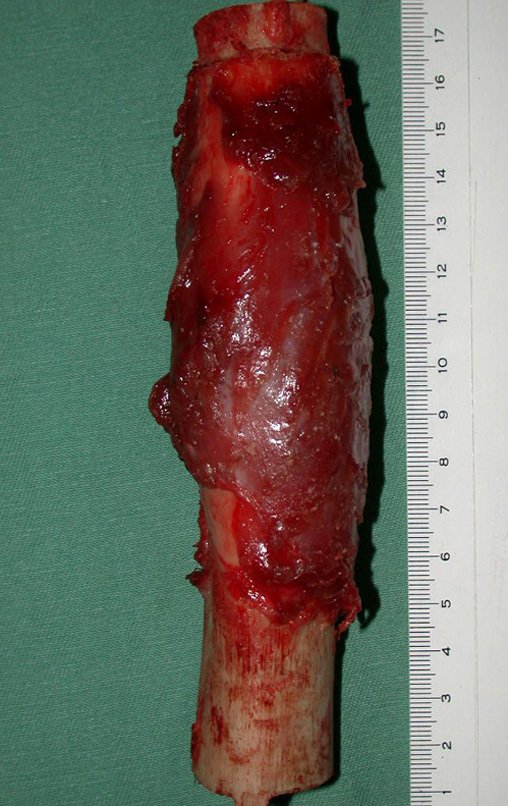
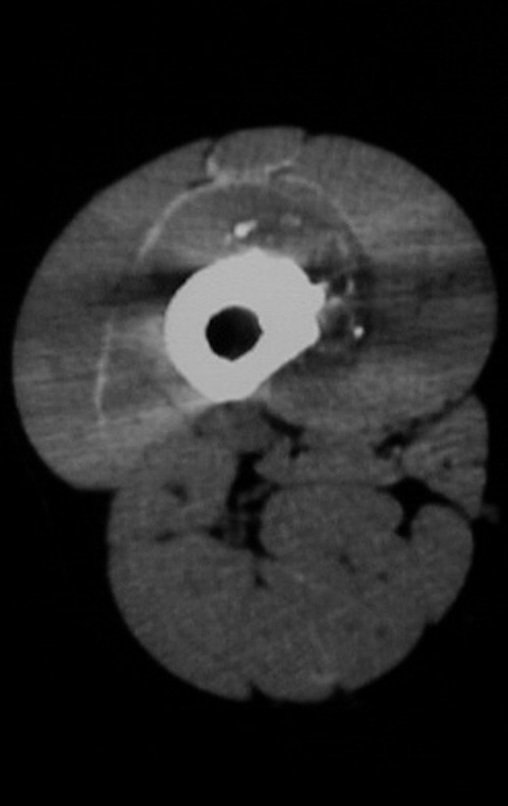
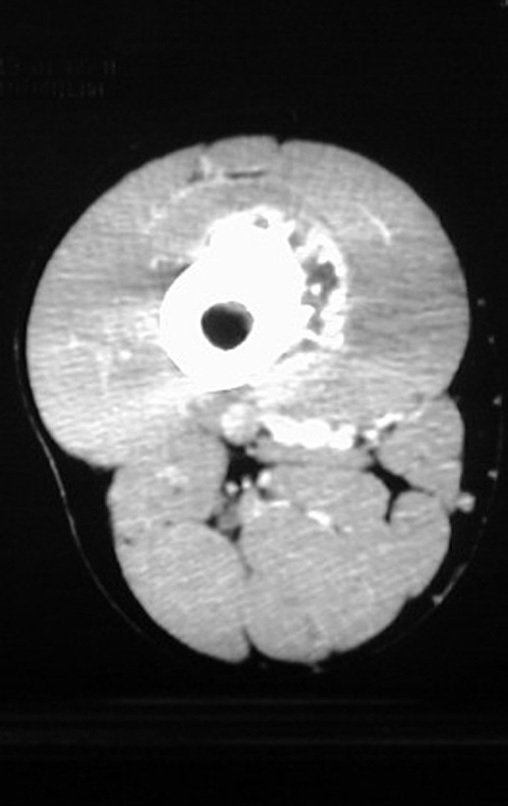
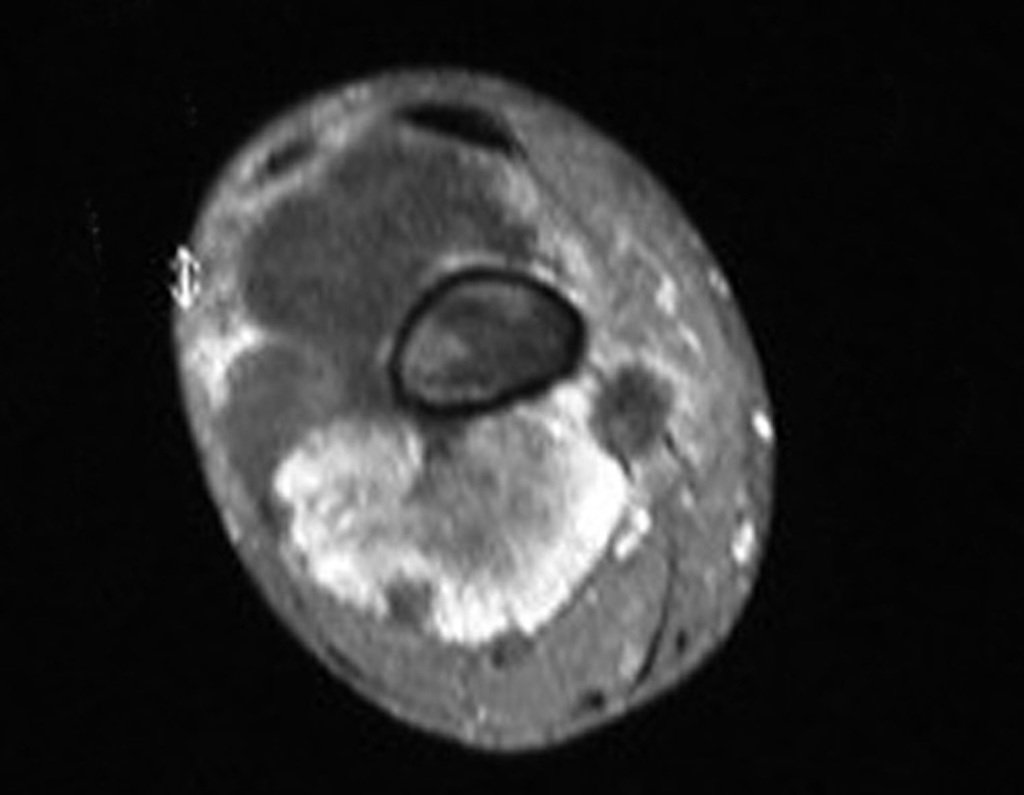
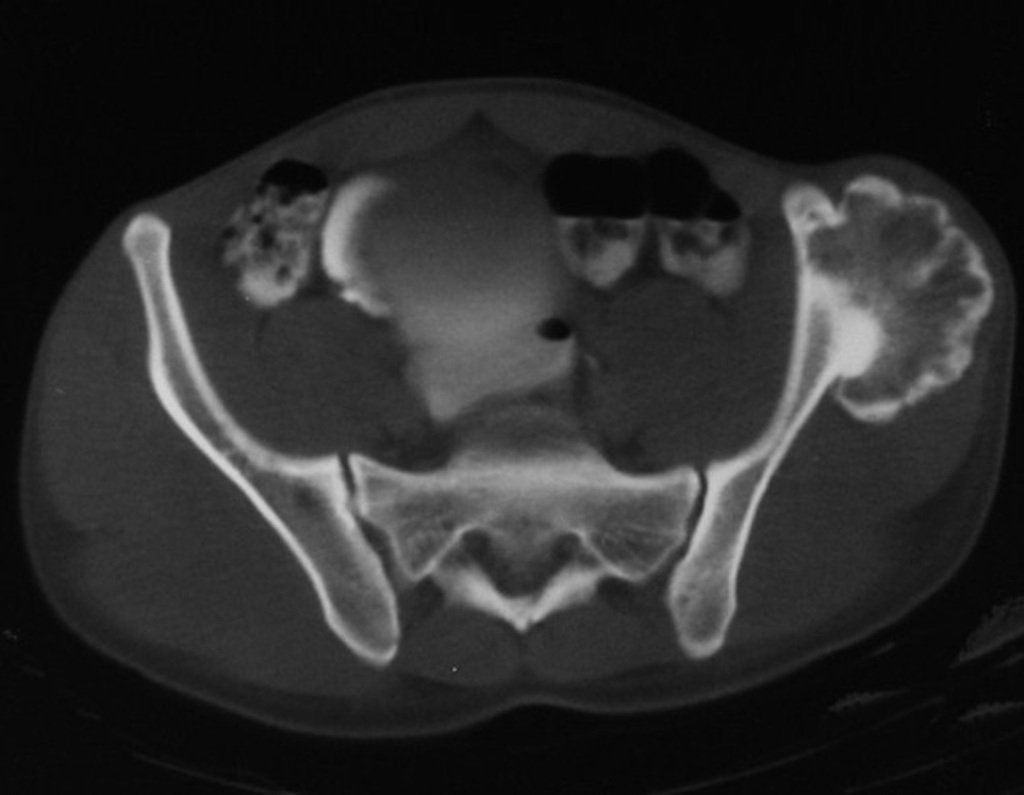
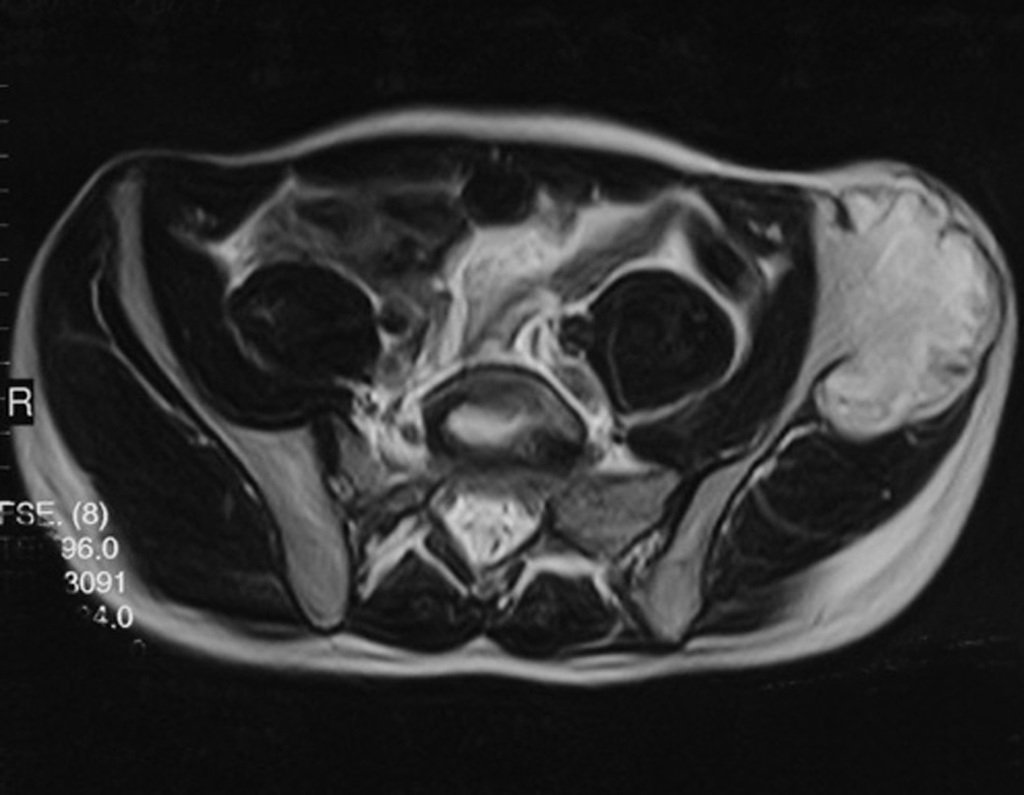
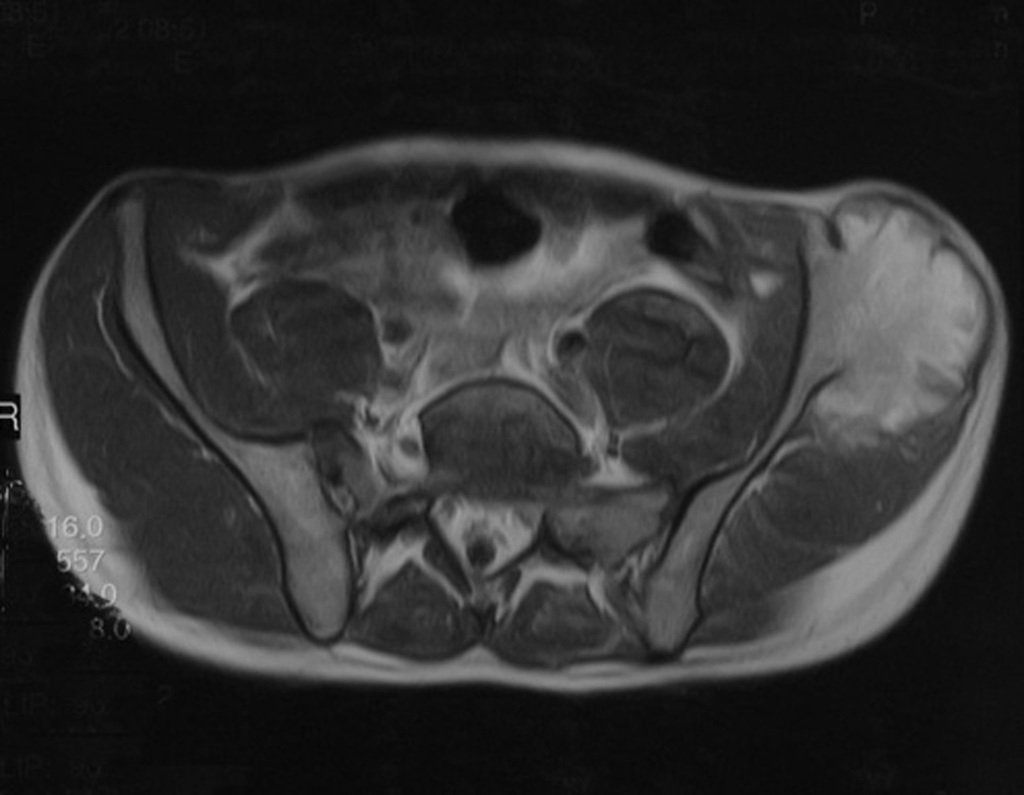
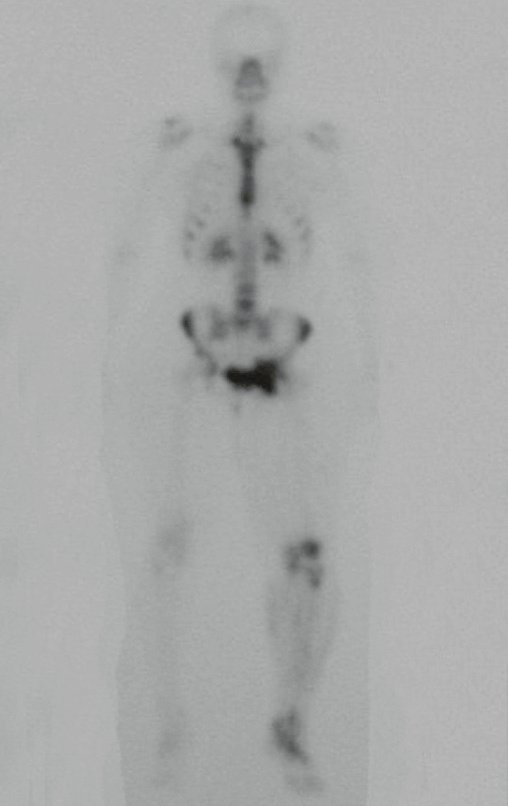
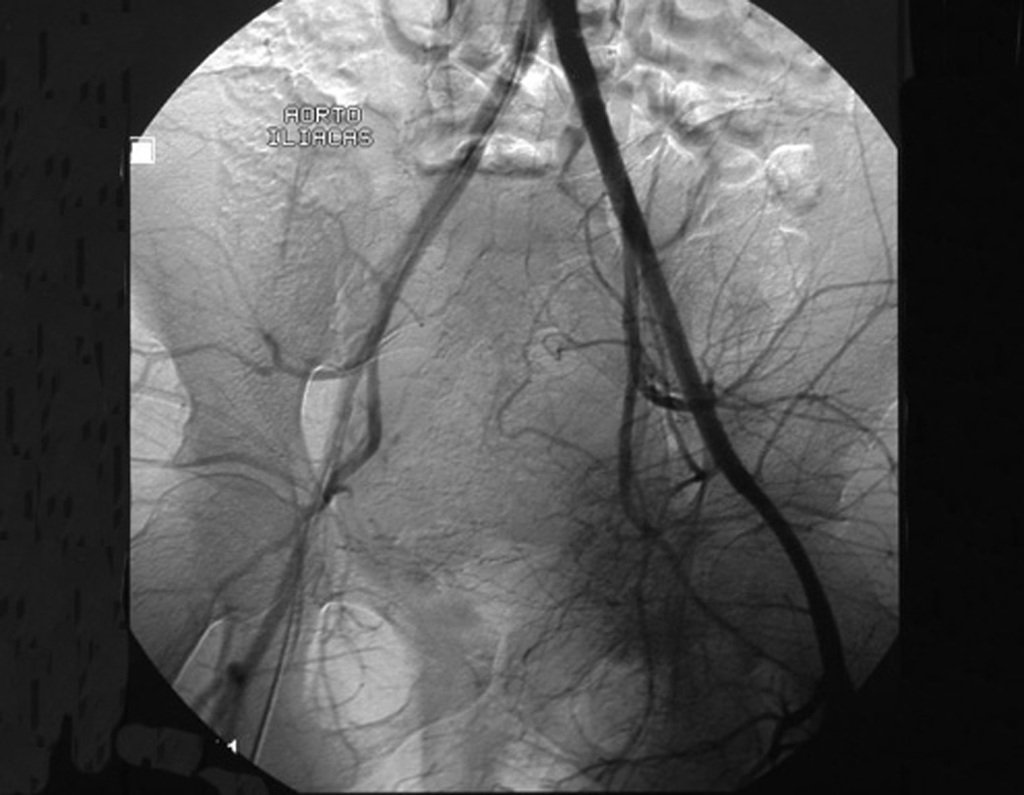
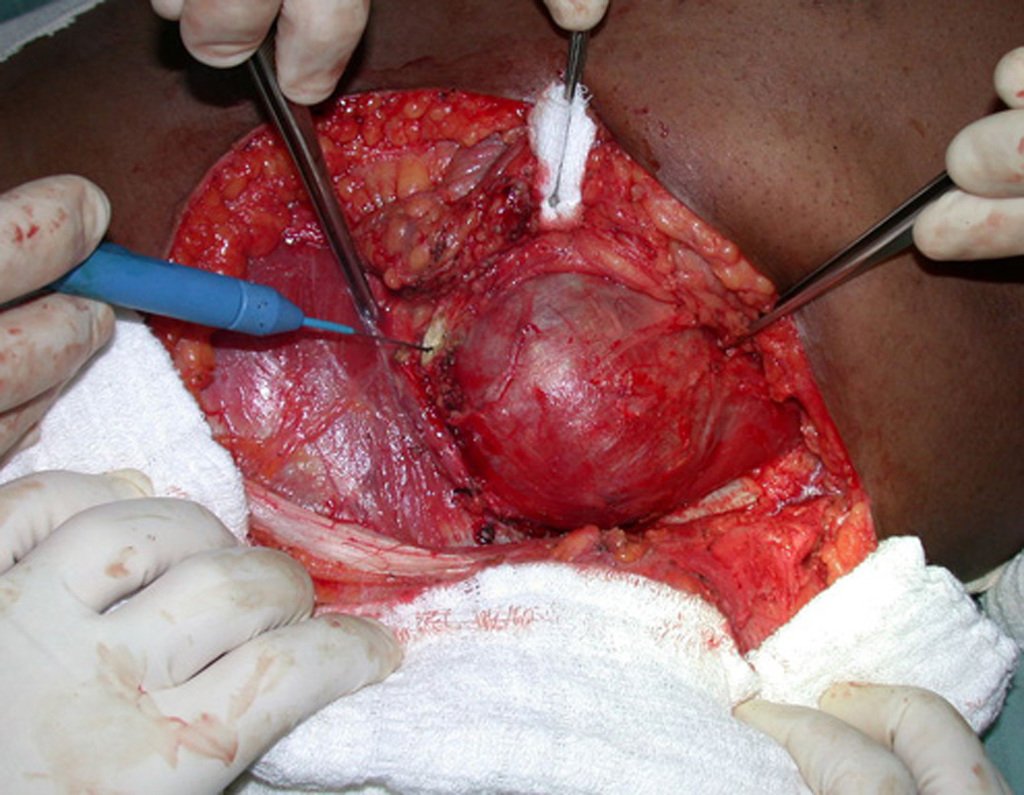
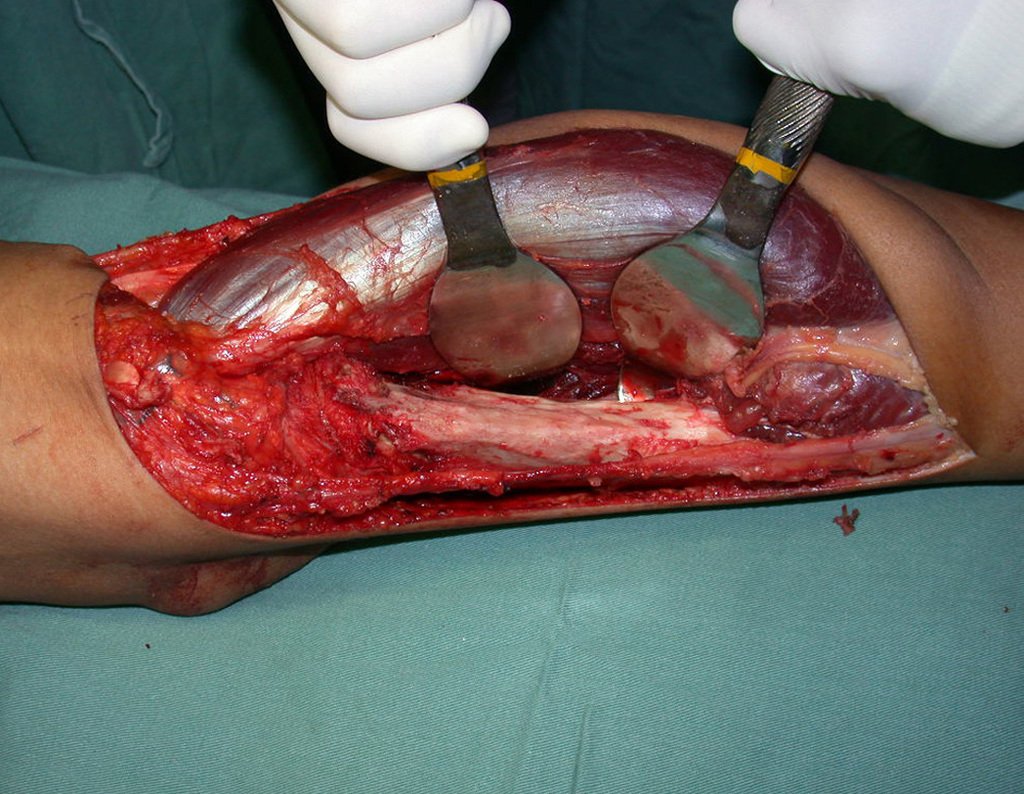
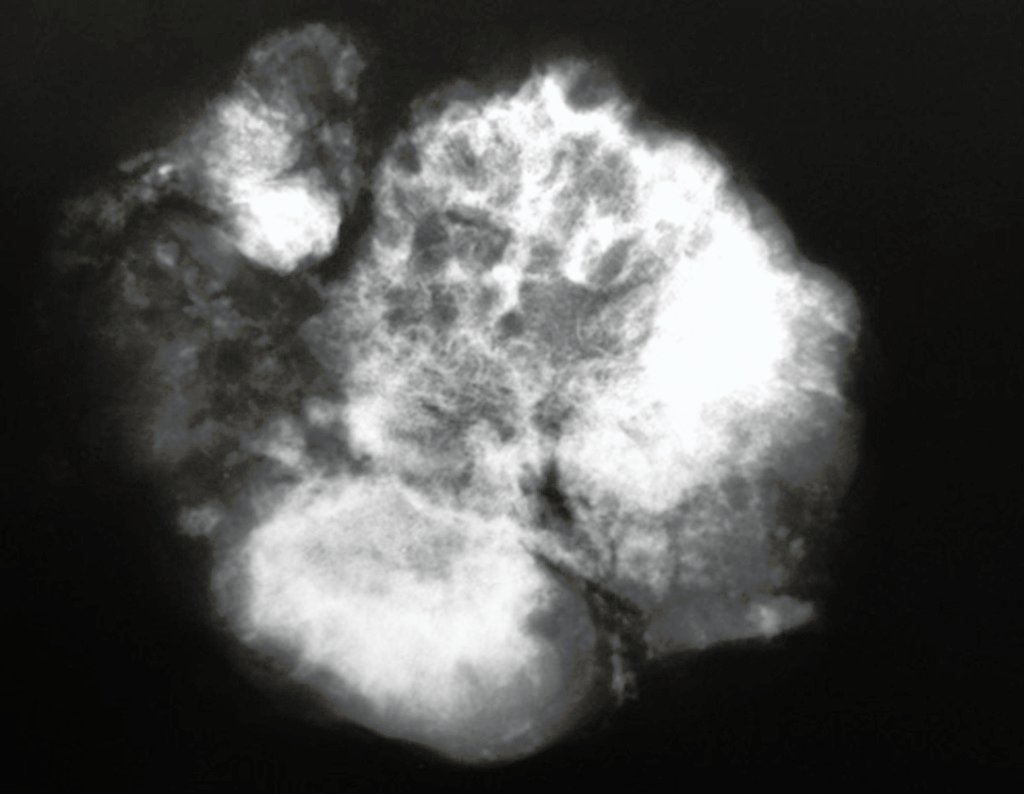
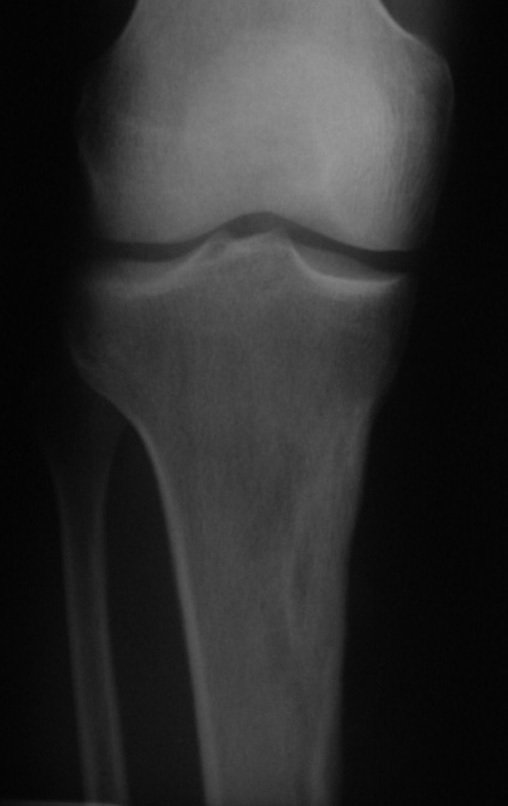
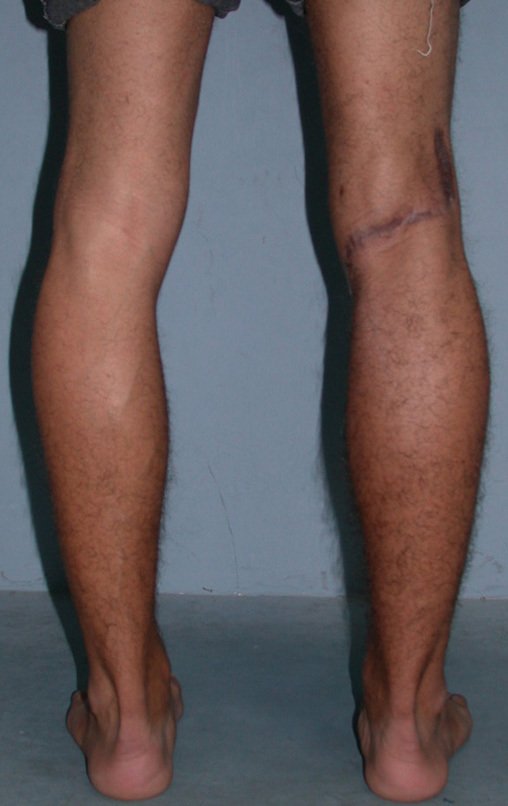
Chondrosarcoma occurs in bones of endochondral origin, mainly in the roots of the limbs: shoulder (Figures 1 to 3), pelvis (Figures 4 to 10), ribs and axial skeleton 1 , being rare in bones of membranous origin 11,14,15 ,24.
In most cases they are painless and do not cause motor deficits. The occurrence of fractures is uncommon 7,10,13,22 and patients seek treatment many years after the appearance of the tumor, as symptoms appear late. Huvos 11 reported a case of rib chondrosarcoma that progressed for fifteen years before the patient sought treatment.
Figures 1 to 10 illustrate large chondrosarcomas of the shoulder girdle and pelvic girdle, which evolved slowly.
Classification: They can be classified according to location, histology and origin.
As for location, they can be:
A- central (Figures 11 to 15);
B- juxtacortical, paraosteal, or periosteal 2,6,23,24 (Figures 16 and 17);
C- peripheral or exophytic , which occurs on an osteochondroma 28 (Figures 18 and 19) and
D- soft tissue 13 (Figures 20 to 31).
Regarding HISTOLOGY , they present different aspects, which can be separated into:
A) Degree of Anaplasia : they are classified into grades I ,
II and III , depending on cellularity and atypical mitoses11,24, being:
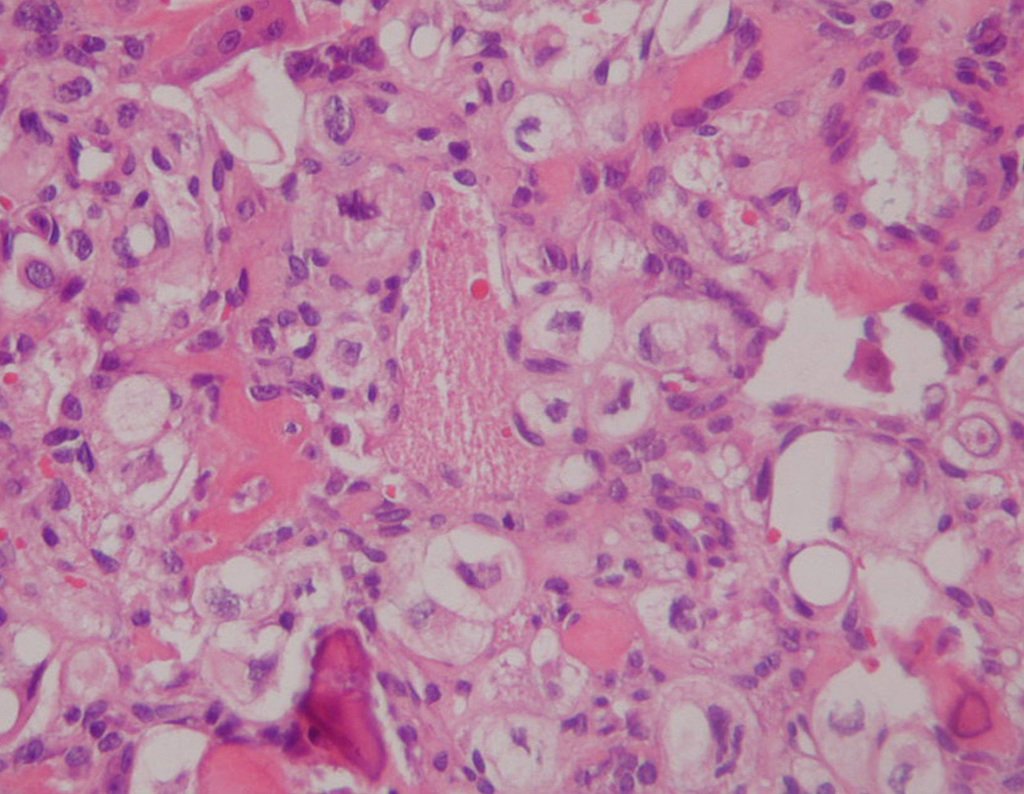
-Chondrosarcoma grade I , well differentiated, similar structure to hyaline cartilage but with increased cellularity, irregular distribution of gaps and a varied number of cells per gap, sometimes binucleate, hyperstained and polymorphic (Figure 10.32);
-Grade II chondrosarcoma , moderately differentiated, greater number of cells due to gaps with great polymorphism and cellular disarray (Figure 10.33);
– Grade III chondrosarcoma , undifferentiated, marked anaplasia, myxoid areas, undifferentiated cells and scarce hyaline matrix (Figure 34).
B) Dedifferentiated : clear areas of mature cartilage and other areas with immaturity, showing high cellularity and atypical mitoses 8 (Figure 35);
C) Mesenchymal : rare, presenting fields of hyaline cartilage interspersed with undifferentiated neoplasia of small, round cells 8 (Figure 36), and
D) Clear Cells : rare, presents round cells with clear or vacuolated cytoplasm and little cellular atypia 2 Figure 37).
As for ORIGIN, they can be:
1- Primary , when it occurs in tissue that had no previous injury (Figures 38 and 39).
2- Secondary , which originates over a pre-existing benign cartilaginous lesion 2,3,6,8,13,14,23,24 (Figures 40 to 44).
Secondary chondrosarcoma occurs in Ollier’s disease or Maffucci Syndrome in 20 to 30% of cases 2,29 , and can also occur as a result of a single enchondroma, although it is rare in this situation.
It can also develop from the cartilaginous layer of a solitary osteochondroma, less than 1%, or multiple osteochondromatosis, around 10% 2 and more rarely secondary to Paget’s disease.
In osteochondroma, when an increase in the lesion is observed after skeletal maturity, the possibility of malignancy must be considered.
This malignancy is characterized by an increase in the thickness of the cartilaginous layer greater than 2 cm29, irregular calcifications, the appearance of pain and a heterogeneous appearance of the lesion2,6 .
Due to the different morphological characteristics and clinical behavior of the chondrosarcoma subtypes, we consider it educational to discuss individually the incidence, clinical, radiographic and anatomopathological aspects of each subtype:
1. Central or Conventional Chondrosarcoma
It is the most frequent of chondrosarcomas, accounting for 90%8. It represents between 10.0 and 14.5% of all primary malignant bone tumors 2,23 .
According to Dahlin and Jaffe, it affects men and women equally, while for other authors there is a male prevalence that varies from 10% 6,9,14,29 to around 70%, according to Schajowicz 2 .
It occurs more frequently in adults between 30 and 60 years old 2,14,24,29.
Its location is most frequent in the proximal segment of the femur, humerus and tibia; being rare in short bones 2,23 .
Pain can be an insidious symptom for several years, evolving with slow growth, increased volume, restricted mobility, with the skin sometimes becoming red and hot 23 . As it is oligosymptomatic, pathological bone fractures are often the first manifestation of the disease 2,24.
The radiograph shows a radio-transparent metaphyseal lesion, replacing the bone marrow. The tumor grows towards the epiphysis or diaphysis and erodes the inner cortex, causing punch-hole lesions. Expansion of the medullary portion of the bone may occur, with cortical inflation (Figures 45 and 46).
The x-ray shows frequent calcifications (Figure 47). This results from the neoangiogenesis of cartilaginous tissue, which degenerates. This process is accelerated in chondrosarcomas and slowed in benign and low-grade cartilaginous lesions. Calcifications can be speckled, cotton flaked or ring-shaped 23,2,24,13,6,29,5 .
Bone mapping helps in tumor staging (Figure 48). Magnetic resonance imaging and tomography are important for evaluating the intramedullary extension and extraosseous involvement of the lesion 2 .
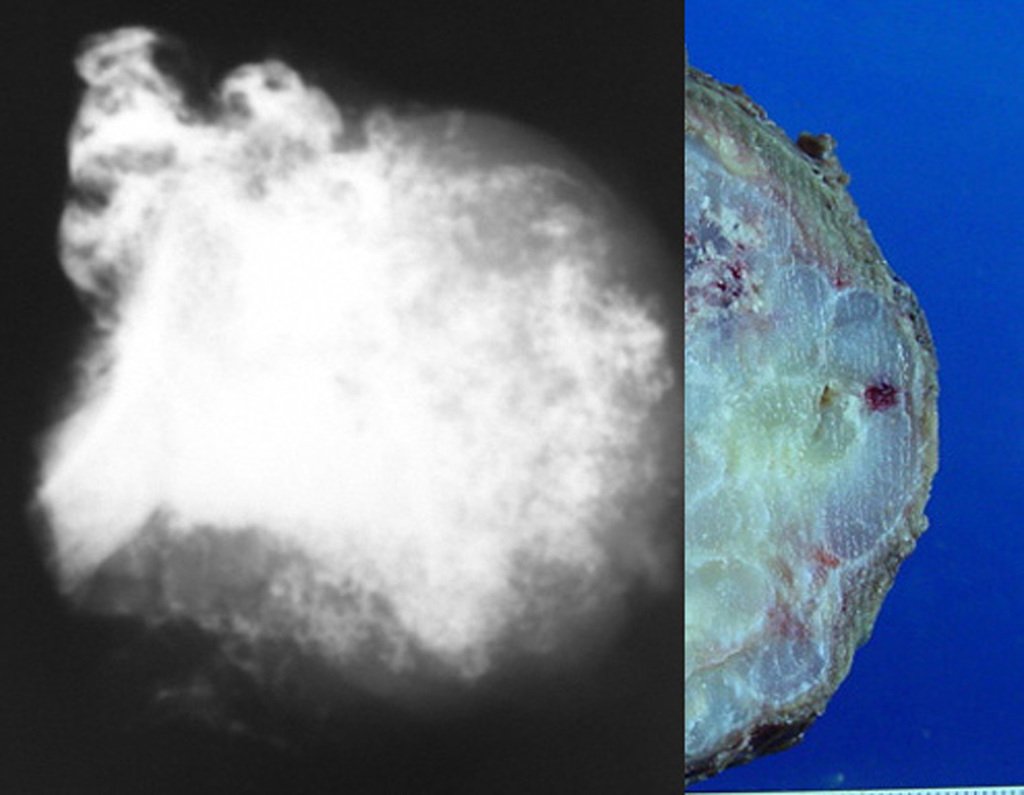
Macroscopy shows a bluish-white color with foci of yellowish calcification, forming lobes separated by connective tissue septa and areas of necrosis 2,24,6,14 (Figures 49 and 50).
Microscopically, central chondrosarcoma presents hypercellularity, bulky nuclei, sometimes binucleate, polymorphism, atypia, myxoid intercellular matrix, invasion and destruction of adjacent bone trabeculae. This histology may also present a low or high degree of dedifferentiation.
Low-grade lesions can be confused with benign cartilaginous tumors, as the histological difference between these tumors is subtle. A low-grade lesion is considered when there is moderate cellularity, atypia, polymorphism and binucleate forms 12 (Figure 51).
At high levels, there is hypercellularity, atypia and marked polymorphism, with several mitotic figures in the myxoid intercellular matrix 14,12 .
2. Juxtacortical (or surface) chondrosarcoma
Also called parosteal or periosteal, these tumors develop on the surface of the bone.
They are rare, representing 20% of chondrosarcomas, in general, they are low grade and occur in young adults 23 . They affect the metadiaphyseal region of long bones, with preference in the posterior and distal region of the femur, anterior and proximal tibia and proximal humerus 14 .
The lesion involves the cortex, with poorly defined margins and grows more quickly than conventional chondrosarcoma. They have a hard consistency, are generally painless and without signs of inflammation on the underlying skin 23 (Figures 52 to 60).
In the highly malignant variable, there is cortical erosion and the presence of a palpable, soft and painful tumor 2 .
Radiographically, a transparent bone rarefaction lesion may occur, with foci of calcification between the eroded bone cortex and the elevated periosteum.
Macroscopically, at diagnosis, it is a lesion larger than five centimeters, lobulated and adhered to the surface of the bone.
Microscopy is similar to conventional chondrosarcoma. Tumor nodules may invade peripheral soft tissues.
3. Peripheral or exophytic chondrosarcoma It differs from the juxtacortical type, as it arises from a pre-existing osteochondroma. Malignancy of an osteochondroma should be considered when the lesion grows after skeletal maturity, without previous trauma or repetitive friction.
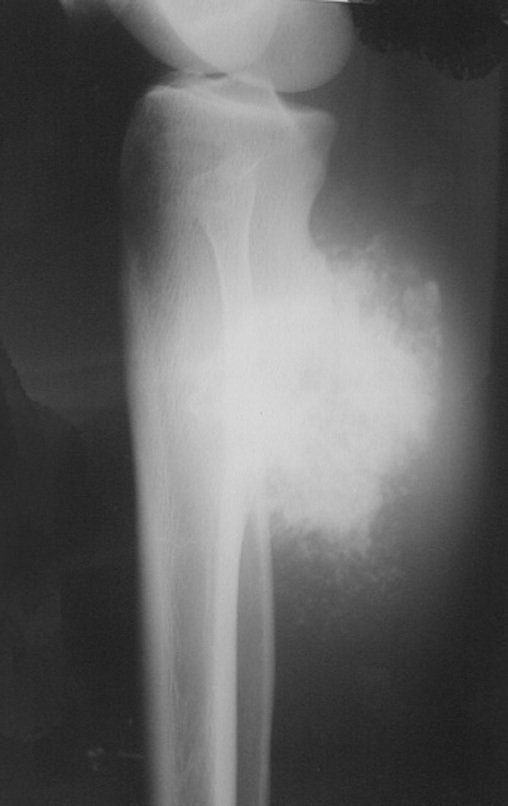
Radiographically, they present large-volume tumors, with radiopaque areas on the periphery, with a globose or ovoid appearance, smooth or multilobulated surface, calcified in the central portion, strongly implanted in the host bone, appearing to be a vegetative tumor, which is not always confirmed, as it has limits well-defined external elements 23 .
They grow more slowly than the central type and are often large at diagnosis 12,14.
This type of chondrosarcoma can only be cured with adequate resection. A parietal resection of the bone portion where the osteochondroma is located must be performed 29,12 , avoiding blunt dissection of the surface of the lesion.
In sarcomatous degeneration, there is an increase in the thickness of the cartilage layer, with irregular calcifications and pain where previously it was painless 2,4 .
They are most common in the ilium and scapula, followed by the proximal region of the femur, distal femur, proximal humerus and proximal tibia 3,12,23,29.
Figures 61 to 103 illustrate examples of peripheral chondrosarcoma, secondary to osteochondroma, with different aspects, in the main frequency locations.

The histological diagnosis of well-differentiated chondrosarcoma is challenging.
The same histological appearance of irregularity in the arrangement and number of cells within the chondroid matrix, with nuclear changes of hyperchromasia, discrete polymorphism and some atypical mitoses, can represent different entities: chondrosarcoma, when located in the roots of limbs, and chondroma when found in the hands and feet.
Under microscopy, the description of chondromas of the hands and feet is similar to that of central chondrosarcoma 23 .
Data on clinical history, location and imaging aspects must be valued to conclude the diagnosis and define appropriate management 12,14,23.
4. Mesenchymal Chondrosarcoma
Initially described by Lichtenstein and Bernstein in 1959 16 , it is extremely rare 24 . The largest case series, thirty cases, was published by Salvador 18 .
It is characterized by areas of differentiated cartilage, interspersed with mesenchymal tissue with round or fusiform cells, highly vascularized with a hemangiopericytic pattern 2 (Figure 104).
It presents a slight predominance in females, occurs between the second and third decades of life 2,6,14 , and frequently appears in the lower extremities, jaws, mandible and ribs. Pain and increased volume are the main clinical symptoms 2.
It may resemble conventional chondrosarcoma.
Radiographically, it has an aggressive appearance 29 with involvement of soft tissues and frequent pulmonary metastases 12.
It presents a high degree of malignancy, with small round or fusiform blue cells surrounding cartilage islands, with a well-differentiated benign appearance, a pattern similar to hemangiopericytoma 24,29 .
The cells resemble undifferentiated chondroblasts 6 .
Macroscopically, they present areas of grayish-white or yellowish color, with a soft consistency, alternating with hardened areas, with a cartilaginous appearance and foci of calcification.
5. Clear Cell Chondrosarcoma
Rare neoplasm, located in the epiphyses of long bones and composed of round cells with abundant, clear cytoplasm and numerous giant cells 2,24 , 29 (Figure 105).
It essentially affects adults and involves the proximal femur, humerus and tibia 2,29 .
On radiography, it appears as a well-defined epiphyseal lesion, similar to a giant cellular tumor (GCT) 2 or chondroblastoma, interpreted by some authors as the malignant evolution of this neoplasm 4 .
Diagnostic doubts regarding chondroma may occur, and radiographic aggressiveness must always be considered to define appropriate management.
6. Dedifferentiated Chondrosarcoma
It is a highly anaplastic sarcoma together with a low-grade malignant chondrosarcoma, presenting an abrupt transition between the two 29 (Figure 106).
It may have the appearance of malignant fibrous histiocytoma, fibrosarcoma, osteosarcoma or rhabdomyosarcoma 2,29 .
It affects the pelvis and long bones, particularly the femur and humerus. It occurs in patients over twenty years of age and has a peak incidence between 40 and 50 years of age, with no predilection between men and women.
On radiography, the lesions are similar to common chondrosarcoma, but the presence of a larger area of cortical lysis suggests an aggressive lesion 29 .
Differential diagnosis:
It presents a differential diagnosis with myositis ossificans, chondromyxoid fibroma, GCT, non-Hodgkin lymphoma 6,23,29 and aneurysmal bone cyst, due to its multiloculated nature. Histologically, the juxtacortical subtype resembles chondroma, osteochondroma, chondroblastoma and surface osteosarcoma 16 .
Clear cell chondrosarcoma has malignant chondrocytes with clear cytoplasm, osteoclast-like giant cells, and intralesional reactive bone formation causing confusion with osteosarcoma.
Mesenchymal chondrosarcoma is formed by islands of well-differentiated hyaline cartilage surrounded by sheets of small, round cells, reminiscent of hemangiopericytoma and Ewing’s sarcoma 14.
Central chondroma of long bones, chondrosarcoma and bone infarction are often difficult to differentiate, requiring clinical and radiographic monitoring to assess whether or not the lesion has progressed, before defining the course of action. Biopsy
is often not definitive for diagnosis 12,23,29.
Treatment:
The treatment of chondrosarcoma is surgical 25 , and a wide resection must be chosen, including the biopsy path 13,21.
Radiotherapy is ineffective 6 in controlling this neoplasm. For high-grade lesions, it is possible to discuss the indication of chemotherapy using the protocol for large cell sarcomas, based on anthracyclines 9999. For mesenchymal chondrosarcoma, which presents a predominance of small and undifferentiated cells, chemotherapy, when indicated, falls under the protocol of treatment of Ewing Tumor. 888
In both cases, the response to chemotherapy is usually poor 6 . The treatment of this neoplasm must be individualized for each clinical subtype:
– Central chondrosarcoma has high cure rates with appropriate surgery, therefore its treatment with intralesional curettage cannot be underestimated, even followed by complementary adjuvant methods, whether with phenol, liquid nitrogen, electrothermia or CO 2 laser 21.
Therefore, in cases of diagnostic doubt between chondroma and grade I chondrosarcoma, it is preferable to observe the evolution of this lesion, as it is known that the biopsy will not be conclusive, as the histological differential diagnosis between chondroma and grade I chondrosarcoma is difficult.
In some cases, these lesions can be treated with conservative surgery without performing a prior biopsy 21 .
When imaging tests: radiography, tomography and magnetic resonance, show a central lesion, without erosion of the internal cortex, with a casual and painless finding, it should be reevaluated initially within three months, if unchanged, repeated within six months and If the lesion remains unchanged, annual reassessments are scheduled.
If, at any time, there is a change in the clinical picture or imaging, it should be treated as central chondrosarcoma, carrying out wide resection of the lesion and reconstruction with non-conventional endoprosthesis, osteosynthesis with autologous or homologous graft or ablative surgery as necessary. of each case.
In the experience of these authors, it is unnecessary to operate on a painless chondroma when it is found casually, without radiographic aggressive characteristics. Performing an intralesional curettage, with local adjuvant and graft or cement, will not eliminate the need for careful observation. If the anatomopathological examination of the entire curettage reveals that it was chondrosarcoma, it will be much worse to re-operate on this region that has already been surgically manipulated.
There are several cases of “chondroma” in which the histology of intralesional curettage corroborated the biopsy appearance of “chondroma” and however had an unfavorable outcome. When monitoring these patients, imaging tests revealed that there was a “new” lesion at the site and that it was now chondrosarcoma.
In these curettages, local and distant dissemination and even dedifferentiation of the chondrosarcoma may occur, significantly worsening the prognosis.
– Juxtacortical chondrosarcoma, treatment is essentially surgical, with partial parietal resection EXAMPLE possible when possible, an effective procedure with lower morbidity compared to segmental resection.
– Peripheral chondrosarcoma , secondary to osteochondroma, care must be taken especially with the surface of the lesion, which presents anaplasia.
The surrounding soft tissue perimysium should be removed as an oncological margin to prevent local recurrence.
It is important to highlight that when there is growth of a bony exostosis after skeletal maturity, heterogeneous calcification, thick cartilaginous cap, unrelated to friction or trauma, it is probably a chondrosarcoma.
In this situation, a negative biopsy sample does not exclude the possibility of malignancy in the remainder of the lesion, and resection surgery with an oncological margin must be performed, paying special attention to the surface of the lesion.
– Mesenchymal chondrosarcoma , in addition to the need for local control with extensive surgery, may eventually be indicated for additional chemotherapy treatment 9999 .
– Dedifferentiated Chondrosarcoma , such as Clear Cell Chondrosarcoma, local control must be carried out with extensive surgery and chemotherapy with cisplatin and doxorubicin 9999.
Complications:
Intralesional curettage of chondrosarcoma can lead to local recurrence of the disease and more aggressive histological dedifferentiation.
In cases of dedifferentiated chondrosarcomas, hematogenous metastases to the lungs are frequent, which may present lymphatic dissemination and local recurrence 29 . Many chondrosarcomas tend to spread locally 14 , reaching enormous sizes and becoming inoperable, causing death due to compression or complications from this local spread.
Local recurrence increases the incidence of lung metastases 21.
Bibliography
1. ACKERMAN, L.V.; SPJUT, HJ Tumors of bone and cartilage. Atlas of tumor pathology. Washington, Air Force Inst. Pathology, 1962, fasc, 4.
2. CANALE, ST Campbell.Barueri orthopedic surgery: Manole; 2006
3. DAHLIN, DC Bone tumors. Barcelona: Ediciones Toray S/A; 1982
4. DORFMAN, HD; CZERNIAK, B. Bone tumors. St Louis, CV Mosby Co., 1997, chap. 7, p.410.
5. EDEIKEN, J.; HODES, PJ Radiological diagnosis of human illnesses. Buenos Aires, Panamericana, 1977, chap. 15.
6. ETCHEBEHERE, M. Malignant cartilaginous tumors: Chondrosarcomas. In: Camargo OP Clínica Ortopédica. Rio de Janeiro: Med si; 2002. p. 753-759
7. FELDMAN, F. Cartilaginous tumors and cartilage-forming tumor like conditions of the caps and soft tissues. In: Diseases of the Skeleton System (Roentgen Diagnosis). Part. 6 – Bone Tumors, New York, Springer-Verlag, 1977, p.177.
8. FLETCHER, CDM, Unni KK, WHO – Merters F. (Eds.): World Health Organization. Classification of Tumors. Pathology and Genetics of Tumors of Soft Tissue and Bone. IARC Press: Lyon 2002.
9. GREENSPAN, A. Orthopedic radiology. Rio de Janeiro: Guanabara; 2001.
10. HENDERSON, ED; Le PAGE, GA Apud FELDAMAN, F. Cartilaginius tumors and cartilage forming tumor like conditions of the bone and soft tissues. In: Disease of the Skeletal System (Roentgen Diagnosis).
Part. 6 – Bone tumors, New York, Springer Verlag, 1977, p.182.
11. HUVOS, AG Bone tumors Diagnosis, Treatment and Prognosis. Philadelphia, WB Saunders Co., 1979, p. 13.
12. JAFFE, HL Tumors and tumoral states of bones and joints. Mexico: La Prensa Medica Mexicana;1966.
13. JESUS-GARCIA, R. – Reynaldo Jesus-Garcia
14. LICHTENSTEIN, L. Barcelona: Talleres Graphics Ibero-Americanos; 1975.
15. LICHTESTEIN, L. Bone Tumor. 4 Ed St. Louis, CV Mosby Co., 1972, chap. 15.
16. LICHTESTEIN, L.; BERNSTEIN, D. Unusual benign and malignant chondroid tumors of bone. Cancer, 12:1142, 1959.
17. MARCOVE, RC Chondrosarcoma: Diagnosis and treatment. In: Orthopedic Clinics of North America. Tumors of the musculoskeletal apparatus. Buenos Aires, Panamericana, 1977, chap. 7.
18. MARCOVE, RC et al. Chondrosarcoma of the pelvis and upper end of the femur. In the analysis of factors influencing survival time in 113 cases. J. Bone Joint Surg., 54A:61, 1972.
19. MARCOVE, RC; SHOJI, H.; HARLEN, M. Altered carbohydrate metabolism in cartilaginous tumors. Contemp. Surg. 5:53, 1974.
20. McFARLAND, GBJr.; McKINLEY, L.M.; REED, RJ Dedifferentiation of low grade chondrosarcomas. Clinic. Orthop., 122:157, 1971.
21. MENENDEZ, LR Orthopedic knowledge update: Updates in orthopedic surgery and traumatology. Barcelona: Ars Medica; 2003.
22. O’NEAL, LW; ACKERMAN, LV Chondrosarcoma of cap. Cancer, 5:551, 1952.
23. PROSPERO, JD Bone Tumors. São Paulo, Roca, 2001, chap. II.
24. ROBBINS. Structural and functional pathology. Rio de Janeiro: Guanabara; 1996.
25. ROMSDAHL, M.; EVANS, H.L.; AYALA, AG Surgical treatment of chondrosarcoma. In: Management of primary bone and soft tissue tumors. Chicago, Year book med. Publisher Inc., 1977, p. 125.
26. ROMSDAHL, M.; Evans, H.L.; Ayala, AG Surgical treatment of chondrosarcoma. In: Management of primary bone and soft tissue tumors. Chicago. Year book med. Publisher Inc., 1977, p.125.
27. SAVIOR, AH; BEABOUT, JW; DAHLIN, DC Mesenchymal chondrosarcoma. Cancer, 28:605, 1971.
28. SCHAJOWICZ, F. Juxtacortical Chondrosarcoma. J. Bone Joint. Surg., 59B:473, 1977.
29. SCHAJOWICZ, F. Tumors y Lesiones Seudotumorales de Huesos y Articulaciones. Buenos Aires: Editora Médica Panamericana; 1982.
30. TORNBERG, DN; RICE, R.W.; JOHNSTON, AD The ultrastructure of chondromyxoid fibroma.Clin. Orthop. Rel. Research, 95:295, 1973.
999. J Clin Oncol 30:abstract 100:23,2012(maluf)
888. Buzaide, AC; Maluf, FC; Rocha Lima, CM
Brazilian Clinical Oncology Manual. Dendrix Edition and Design ltda. São Paulo (XI) Adult Bone Sarcomas, 560-79. 2013
Author: Prof. Dr. Pedro Péricles Ribeiro Baptista
Orthopedic Oncosurgery at the Dr. Arnaldo Vieira de Carvalho Cancer Institute
Office : Rua General Jardim, 846 – Cj 41 – Cep: 01223-010 Higienópolis São Paulo – SP
Phone: +55 11 3231-4638 Cell:+55 11 99863-5577 Email: drpprb@gmail.com